Afterload refers to the resistance the left ventricle encounters as it tries to eject blood. Afterload is only conceptual and cannot be measured directly.
Afterload is affected mainly by:
- ventricular volume (size)
- arterial vasomotor tone (arterial resistance)
- ventricular wall thickness
Afterload is increased by:
- increase in ventricular volume
- increase in arterial vasomotor tone
- decrease in ventricular wall thickness
Afterload is decreased by the opposite changes.
How do changes in afterload change cardiac performance?
As afterload increases, stroke volume falls and vice versa. However, changes in afterload have a more marked influence on stroke volume in the failing heart vs the normal heart.
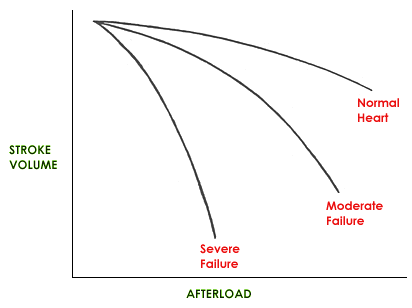
An increase in afterload also increases myocardial oxygen consumption. A reduction in afterload has the opposite effect.
The ability to improve cardiac output by reducing afterload represents a major therapeutic advance for many cardiovascular diseases in the last several decades.
How are changes in afterload detected on physical examination?
Afterload cannot be directly measured. However, we can infer that afterload changed if there is evidence that ventricular volume, ventricular wall thickness, or peripheral arterial resistance changed. In most clinical situations we attempt to infer whether afterload is increased or decreased. One can expect that peripheral arterial resistance (and therefore afterload) is elevated in most cases of heart failure (reduced cardiac output) because of 2 facts:
- Blood Pressure = Cardiac Output x Arterial Resistance
- The body attempts to maintain blood pressure by changing arterial resistance (increasing arterial resistance) in heart failure.
Therefore, if we can infer a fall in cardiac output on physical examination, we can expect a rise in arterial resistance and therefore afterload. The following findings on physical examination may indicate reduced CO, and increased afterload may accompany these findings:
- cool extremities, fall in rectal temperature
- weakness
- slow capillary refill time (>2 sec)
- arrhythmias
- reduced mentation/confusion
- congestive failure signs usually coexist with a reduction in cardiac output
