Cardiovascular system response to circulatory failure
So-called failure may be due to two causes: 1. Circulatory failure due to a lack of circulating volume usually due to blood loss and shock occurs. 2. A failure on the part of the heart to produce enough CO due to heart disease.
In both cases BP falls.
All disorders that result in a fall in BP are addressed by “so-called compensation” on the part of the circulatory system as if the cause for this drop in BP was due to blood loss and reduced preload and the development of shock.
Response of the circulatory system in the case of shock
- Activation/augmentation of the sympathetic nervous system causing:
- An increase in HR – which increases CO
- An increase in contractility – which increases SV
- An increase in arterial vasomotor tone (systemic arterial resistance) – which helps bring BP back to normal
- An increase in venomotor tone – which increases preload (the fundamental abnormality)
- Activation of renin release and thus RAAS activation
2. Activation of the Renin Angiotensin Aldosterone System (RAAS):
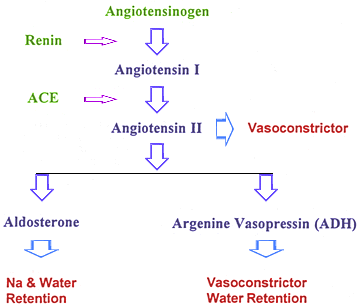
- The production of angiotensin II which causes:
- An increase in arterial vasomotor tone (systemic arterial resistance) – which helps bring BP back to normal
- An increase in venomotor tone – which increases preload (the fundamental abnormality)
- Activates the Arginine Vasopressin (Antidiuretic hormone) which causes:
- An increase in arterial vasomotor tone (systemic arterial resistance) – which helps bring BP back to normal
- An increase in water retention at the level of the kidney – which increases preload (the fundamental abnormality)
- The production of aldosterone which causes:
- Water retention at the level of the kidney – which increases preload (the fundamental abnormality)
3. Increased thirst – which increases preload
4. Redistribution of cardiac output to coronary and cerebral vascular beds and away from:
- cutaneous vascular beds causing
- pale mucus membranes
- slow capillary refill time
- cool extremities
- splanchnic vascular beds causing
- impaired intestinal absorption
- ischemic bowel with ulceration and hemorrhage
- renal vascular beds causing
- reduced GFR
- sodium retention and water retention
WHY the shock response is counter productive for cases of cardiac disease
The response the circulatory system introduces for a true case of shock is intended to support the circulatory system for a time period measured in hours.
The so-called shock response was never intended to support a circulatory system in need of support for a time period measured from days to years.
In the setting of heart failure resulting in a fall in blood pressure, the “shock response” is activated for a period of days to years.
HOW the shock response is counter productive for cases of cardiac disease
Sustained activation of the sympathetic nervous system is detrimental:
- The increase in HR causes increase in MVO2 and reduction in time for ventricular filling and coronary perfusion (during diastole).
- The increase in contractility causes an increase in MVO2.
- The increase in arterial vasomotor tone (systemic arterial resistance) causes an increase in afterload which reduces SV and increases MVO2.
- The increase in venomotor tone increases preload, promoting further pulmonary edema, pleural effusion, ascites, and organ edema.
- Activates renin and thus RAAS which is detrimental (see below).
- Promotes arrhythmias producing dyssynergy of contraction.
- Promotes coronary arterial spasm, leading to ischemia and myocardial necrosis.
Sustained activation of the RAAS is detrimental.
The sustained production of angiotensin II causes:
- The increase in arterial vasomotor tone (systemic arterial resistance) causes an increase in afterload which reduces SV and increases MVO2.
- The increase in venomotor tone increases preload promoting further pulmonary edema, pleural effusion, ascites, and organ edema.
- Angiotensin II triggers signaling pathways leading to myocardial necrosis.
- Activates the Arginine Vasopressin (Antidiuretic hormone) causing:
- An increase in arterial vasomotor tone (systemic arterial resistance) – causes an increase in afterload which reduces SV and increases MVO2.
- An increase in water retention at the level of the kidney, which increases preload promoting further pulmonary edema, pleural effusion, ascites, and organ edema.
The sustained production of aldosterone causes:
- Water retention at the level of the kidney, which increases preload promoting further pulmonary edema, pleural effusion, ascites, and organ edema.
- Causes myocardial and vascular fibrosis
Increased thirst is detrimental because it increases preload which promotes further pulmonary edema, pleural effusion, ascites, and organ edema.
Thus sustained activation of these “so-called compensatory” measures accelerates the demise of the patient with a dysfunctional heart as the cause for the reduction in BP. Thus activation of the shock response for a time period measured in hours is supportive. Activation of the shock response for a time period measured in days to years is detrimental.
