Auscultation remains the most useful and expedient assessment of the cardiac patient. When combined with the signalment and history, it can often provide a strong differential diagnosis list and in rare instances a near definitive diagnosis in very experienced hands (ears!).
The goals of cardiac auscultation include:
- To determine the heart rate
Bradycardia, normal, or tachycardia
| Species | Normal In-Hospital Heart Rate Range |
| Dog | 60-160 bpm |
| Cat | 120-220 bpm |
2. To determine if there is a rhythm disorder
To be distinguished from a normal sinus arrhythmia
3. To determine if there are abnormal extra heart sounds
- Heart murmurs
- Gallop sounds: S3 or S4 or summation
- Systolic clicks
- Split heart sounds: split S1 or S2
- Pericardial friction rubs – rare in small animals
4. To determine if there are muffled or absent heart sounds
This may occur due to insulation between sound source and stethoscope as in:
- Presence of fluid in the pericardial space = pericardial effusion
- Presence of fluid in the pleural space = pleural effusion
- Mass in the pleural space or pericardial space
- Pleural tumors
- Pericardial tumors
- Diaphragmatic hernia either to the pleural or pericardial space
- Lung parenchymal disease
- Obesity
May be a normal variant in some dogs.
Prior to auscultation, consider cardiac palpation (precordial palpation). Precordial palpation is useful to:
- detect a thrill – a thrill refers to a vibration on the chest wall due to fluid turbulence within the heart that also causes a heart murmur on auscultation. Only the very loudest heart murmurs will be accompanied by a thrill
- detect dysrhythmias
- detect suspicion of cardiomegaly
- confirm location of apex beat – usually on left – some disorders will cause the apex beat to shift to the right chest wall
Technical aspects about stethoscopes and auscultation
An important aspect of auscultation is understanding the tool, the stethoscope, and its proper use.
The stethoscope is composed of ear pieces connected via ear tubes and flexible tubing to a chest piece.
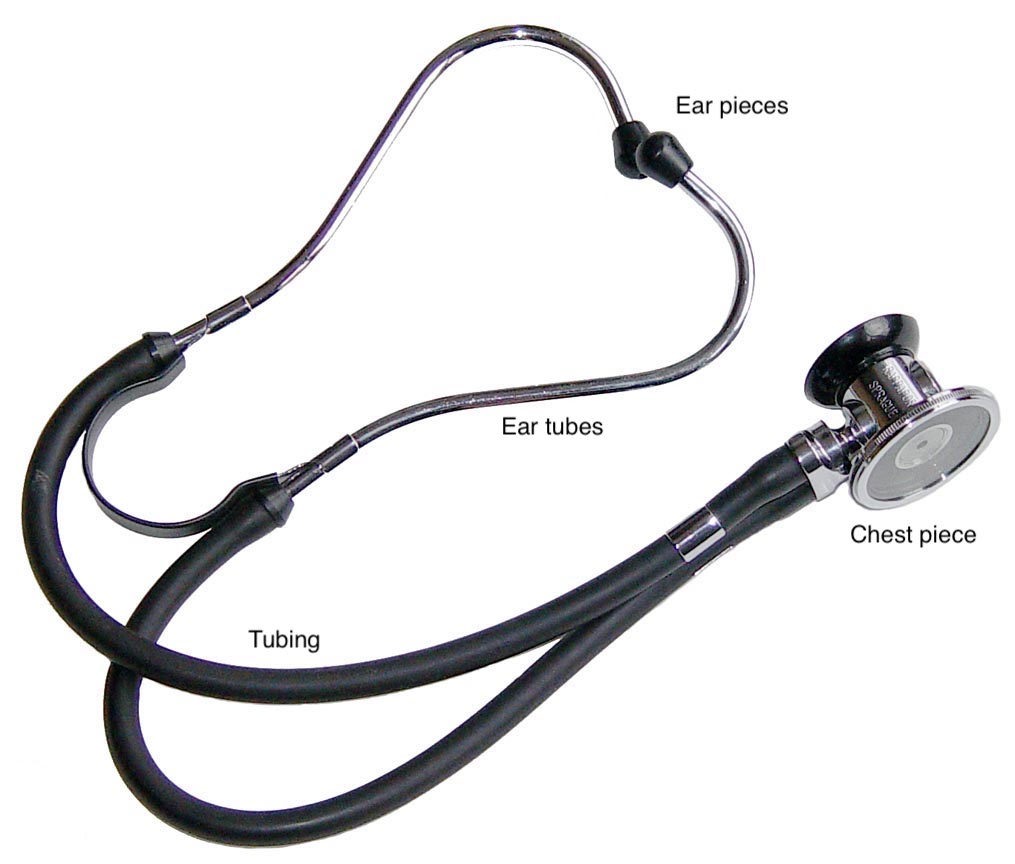
The ear pieces are meant to create a seal in the listener’s ear canal, reducing ambient noise and allowing proper sound transmission from the chest piece to the ears. The ear tubes should be rotated forwards to be in line with the natural direction of the ear canals, and the ear buds (which come in a variety of sizes and materials) should fit snugly in the ear canal to make a tight seal, yet not too tight so as to block the ear canal.
The tubing transmits the sound from the chest piece to the ear pieces. The tubing may be:
- double lumen, where there are two separate tubes from the chest piece all the way to the ear pieces
- single lumen, where there is one tube from the chest piece which then splits to either ear piece
Note that many modern day double lumen stethoscopes have the two tubes encased in one outer tube from the chest piece, so it’s not always easy to tell from the outside which model is double vs single lumen!
Double lumen 
Also double lumen! 
Single lumen
Which do you think is more sensitive and has better sound reproduction? You got it, double lumen. That does come at a higher price tag, but it’s worth it!
A final note about tubing – some models are available with different tubing lengths. Shorter tubing will have better sound transmission. Longer tubing may be desirable for large animal work.
Now on to the chest piece. The chest piece is composed of a diaphragm and a bell. The chest piece is rotated 1800 to activate the desired side for use on the chest.

- The diaphragm is best to listen to higher frequency sounds (which includes most heart and lung sounds in small animals)
- The bell is best to listen to lower frequency sounds like gallops

Some stethoscopes have only one side to the chest piece which acts as a “tunable” diaphragm, where with light pressure it is intended to act as a bell and with more firm pressure as a diaphragm. This may work well on fur-less humans, but maybe not as well on our furry patients.
Optimize your listening conditions
A lot of heart sounds will fall out of our human-capable audible range (which is about 20 – 20,000 Hz). So to detect the ones we have a chance to hear, we need to put all conditions in our favour. These include:
- Quiet room, cooperative patient, and thorough exam!
- Have a capable handler to help hold the patient’s head and close the mouth if needed if panting.
- Choose a quiet exam room instead of the middle of the busy treatment area or ICU.
- Don’t be shy to ask other people in the room to be quiet.
- Try to always listen to patients while they are standing. Sitting is acceptable if they won’t remain standing, but standing is preferred. Do not listen while they are in sternal or in lateral recumbency – sounds may be masked or falsely created.
The Harsh Reality
So you’ve got your shiny new double lumen stethoscope, a quiet room, and a cooperative patient. Why are you still not sure what you’re hearing? It’s called experience and practice, practice, practice. A veterinary cardiologist with the crappiest stethoscope in a loud room will still outperform a first year student with the best stethoscope money can buy in an insulated room. At least I think so… Auscultation is a skill mastered only through repetition and feedback (being told what you’re hearing) for sound recognition. Even listening to high quality recorded heart sounds will achieve this. So listen, listen, listen to everything you can! And get feedback on what you’re hearing by someone with more experience than you.
Happy listening!
