Can radiography diagnose heart failure and how?
Radiography cannot detect a reduction in cardiac output for the needs of the tissue (heart failure) but can provide evidence of pulmonary congestion to suggest congestive heart failure (pulmonary venous engorgement, pulmonary interstitial edema, and obscuring and enlargement of the cardiac silhouette).
Radiography provides the most readily available means to identify pulmonary edema and pulmonary venous congestion. Because the vast majority of cases of pulmonary edema are due to congestive heart failure – then the finding of pulmonary edema is strong evidence of congestive heart failure.
Since pulmonary venous congestion (distention) will/must occur prior to the development of cardiogenic pulmonary edema, to identify the presence of pulmonary venous congestion is also strong evidence of congestive heart failure.
What are the radiographic features of pulmonary venous distention and pulmonary edema?
Radiographic criteria of pulmonary venous distention:
- On the lateral view the pulmonary veins to the cranial lung lobes are greater than 75% the width of the proximal 1/3 of the fourth rib
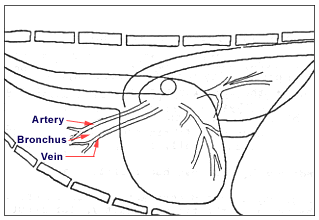
- The pulmonary vein to the cranial lung lobe is obviously larger than its accompanying pulmonary artery (normally they are of equal width)
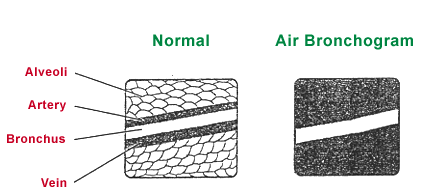
Pulmonary edema refers to an abnormal accumulation of fluid in the interstitium and/or the alveoli of the lungs. As fluid weeps out of the capillaries, at first it accumulates in the perivascular and peribronchial interstitial spaces (producing silhouetting of the vessels, and/or peribronchial pattern on radiographs). Continued fluid accumulation results in edema of alveolar walls and ultimately, alveolar edema (producing air-bronchograms or coalescent [so called cotton-like] pulmonary densities).
Although alveolar edema is usually preceded by interstitial edema, many clinical cases represent a mixture of interstitial and alveolar edema.
Radiographic Appearance:
- Venous engorgement – distention of the veins.
- Interstitial edema – shows a clouding (or silhouetting) of the pulmonary vasculature (perivascular pattern). The walls of the pulmonary vessels are obscured by edema fluid. A peribronchial pulmonary pattern (the most common sign of interstitial edema noted in the dog) also may occur as noted. This pattern is characterized by thickened airway walls. Normally the airway walls are not discernible radiographically after the third generation bronchi due to the lack of cartilaginous support. We typically infer the presence of a bronchus due its position between the artery and vein that lie on each side. The prominent appearance of airway walls throughout the lungs indicates a peribronchial lung pattern, which implies a cellular and/or fluid accumulation in the walls rendering them visible. On cross-section the airway walls are “donut-like”, on long axis view they are “railway tracks-like.”
- Alveolar edema – (flooding of air spaces) shows as coalescing fluffy densities and/or air-bronchograms.
Location of edema:
- Dog: Appears first in the central perihilar area progressing outward and caudodorsally. There is also a high incidence of edema in the anterior ventral area on the lateral view.
- Cat: Variable distribution often occurring in a patchy, irregular pattern primarily in the caudal lobes.
Schematic Of An Air Bronchogram vs A Peribronchial Pattern
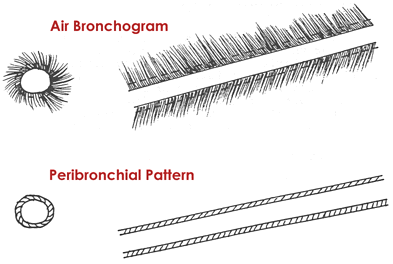
Note how the lumenal wall is readily identified in both examples, but the outside wall is obscured with air-bronchograms.
What other cardiac abnormalities can be diagnosed by radiography?
Radiography can also assist in the diagnosis of:
- chamber enlargement
- great vessel enlargement
- heartworm disease
- pericardial effusion or pleural effusion
